PROFESSIONALS
EXPANDED INDICATIONS
TO RELIEVE OSTEOARTHRITIS
PAIN IN THE:
Knee
Hip
Shoulder
Ankle
PROFESSIONALS
Knee
Hip
Shoulder
Ankle
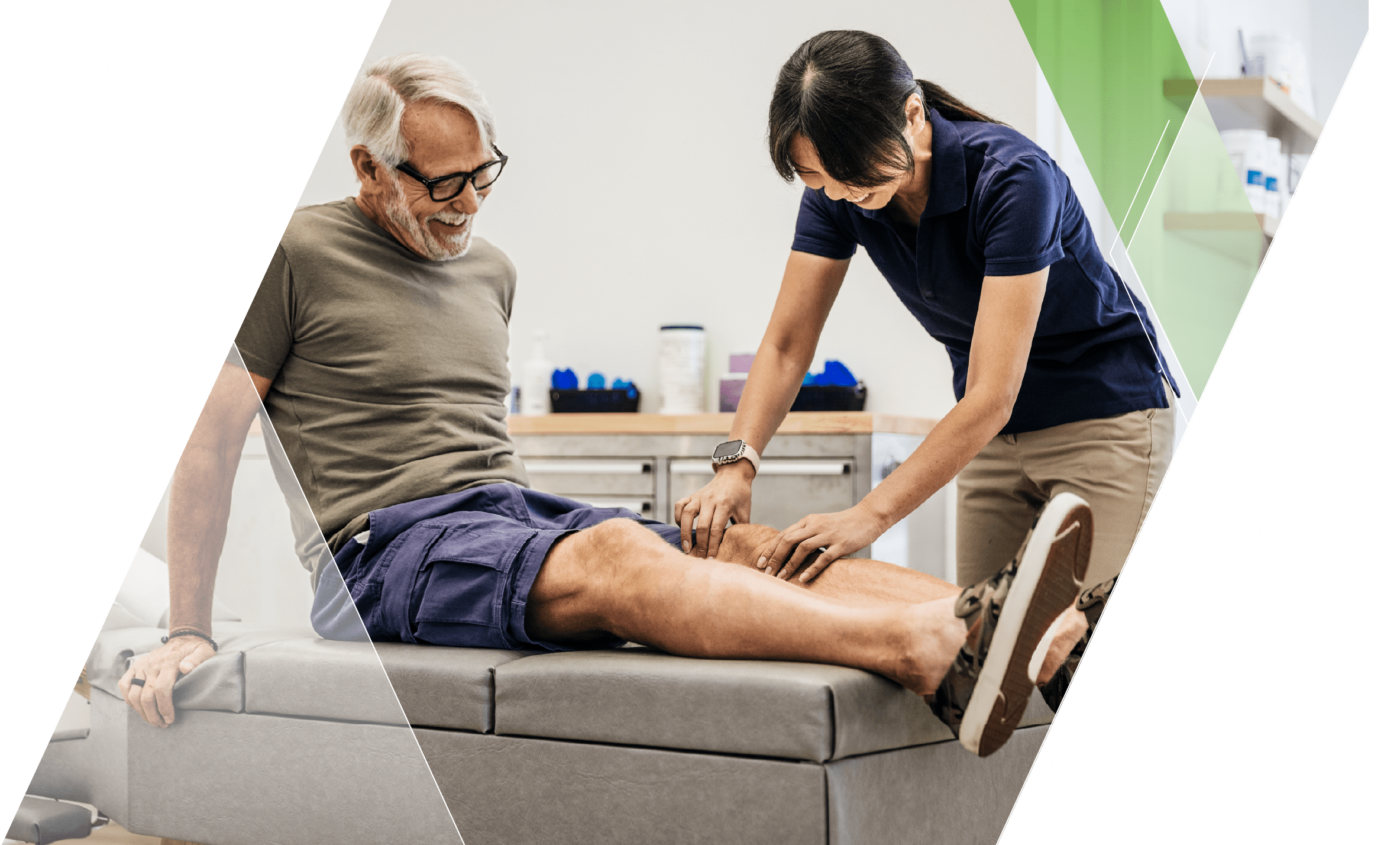
Monovisc® is indicated in the treatment of pain in OA of the knee, hip, shoulder and ankle for patients who have failed to respond adequately to conservative non-pharmacologic therapy and to simple analgesics, e.g., acetaminophen.1

Comparative clinical significance has not been proven.

Percent reduction of WOMAC pain score in the knee from baseline with Cingal®, Monovisc®, or saline in the ITT population**,††,‡‡,6,7


Safety measures
Five serious adverse events were reported in four subjects. None were considered related to treatment and all were resolved without sequelae.
The most common adverse events were headache, arthralgia, spinal pain, back pain, and nasopharyngitis. Six were related to study medication: arthralgia with Cingal® (n=2) and Monovisc® (n=2), peripheral edema with Cingal® (n=1), and rash with Monovisc® (n=1).
Responder rate at 6 months¶¶,3–5,7

Total HA per syringe; single-injection viscosupplements

EXCELLENT SAFETY
PROFILE ACROSS ALL INDICATIONS*,†,‡,§,3–5,7
Contraindications:
Relevant warnings and precautions:
For more information:
Please consult the Monovisc® Package Insert for important information relating to adverse reactions and directions for use that has not been discussed in this piece, or visit www.monovisc.ca.
The Package Insert is also available upon request by calling 1-888-550-6060 or by emailing [email protected] .
References:
1. Monovisc® Package Insert. PENDOPHARM. March 2025.
2. Petterson S, Plancher K. Single intra-articular injection of lightly cross-linked hyaluronic acid reduces knee pain in symptomatic knee osteoarthritis: a multicenter, double-blind, randomized, placebo-controlled trial.
Knee Surg Sports Traumatol Arthrosc
2019;27(6):1992–2002.
3. Data on file. PENDOPHARM. Monovisc® 18-01 Clinical study report.
4. Data on file. PENDOPHARM. Monovisc® 18-02 Clinical study report.
5. Data on file. PENDOPHARM. Monovisc® 18-03 Clinical study report.
6. Hangody L, et al. Intraarticular injection of a cross-linked sodium hyaluronate combined with triamcinolone hexacetonide (Cingal®) to provide symptomatic relief of osteoarthritis of the knee: a randomized, double-blind, placebo-controlled multicenter clinical trial.
Cartilage
2018;9(3):276–283.
7. Data on file. Clinical Study Report: Cingal 13-01.
8. Compendium of Pharmaceuticals and Specialties. Synvisc-One® Product Monograph. Genzyme Canada Inc. March 2, 2009. Synvisc-One® is a registered trademark of Genzyme Corporation, U.S.A.
9. Durolane® website. Available from: www.durolane.com. Accessed on: January 13, 2014. Durolane® is a registered trademark of Galderma S.A., Switzerland.
10. Electronic Compendium of Pharmaceuticals and Specialties. NeoVisc® Product Monograph. Tribute Pharmaceuticals Canada Inc. Accessed on: March 5, 2014. NeoVisc® is a registered trademark of Tribute Pharmaceuticals Canada Inc., Canada.
11. Baczkowicz D, et al. Effects of viscosupplementation on quality of knee joint arthrokinematic motion analyzed by vibroarthrography.
Cartilage
2021;12(4):438–447.
12. Faivre J, et al. Crosslinking hyaluronic acid soft-tissue fillers: current status and perspectives from an industrial point of view.
Expert Rev Med Devices
2021;18(12):1175–1187.